 An estimated 7.5 million Americans have psoriasis, and approximately one-half of that number will have an outbreak of scalp psoriasis at some point psoriasis is a non-contagious, chronic disease, with flare-ups typically interspersed with periods of remission or times when the condition is less active. The name comes from the Greek word for "itch." Once a person has psoriasis, it is very likely that he/she will have it forever. Symptoms may go away and come back. It might respond to various treatments, and it may not. In a nutshell, psoriasis is the body overproducing skin cells. People may have too many skin cells in one location which is why it often swells up, becomes dry and even flaky. It can often be very itchy, red, sore, cracked and very tender. Psoriasis usually affects the scalp, hands, stomach, knees, feet, and elbows. It is linked to dandruff and unfortunately to some forms of arthritis.
An estimated 7.5 million Americans have psoriasis, and approximately one-half of that number will have an outbreak of scalp psoriasis at some point psoriasis is a non-contagious, chronic disease, with flare-ups typically interspersed with periods of remission or times when the condition is less active. The name comes from the Greek word for "itch." Once a person has psoriasis, it is very likely that he/she will have it forever. Symptoms may go away and come back. It might respond to various treatments, and it may not. In a nutshell, psoriasis is the body overproducing skin cells. People may have too many skin cells in one location which is why it often swells up, becomes dry and even flaky. It can often be very itchy, red, sore, cracked and very tender. Psoriasis usually affects the scalp, hands, stomach, knees, feet, and elbows. It is linked to dandruff and unfortunately to some forms of arthritis.
Though research is still inconclusive about the causes of psoriasis, doctors do know that there are specific lifestyle factors that can trigger psoriasis or make symptoms worse. There are many found "triggers" for the skin condition, including drinking alcohol, being overweight, stress, and a lingering case of strep throat, anxiety, some medicines, and sunburns. In about 32 percent of psoriasis cases, there's a family history of the condition, which means there is a significant genetic link. Everyone has a different set of triggers ranging from diet to stress management and according to the Mano Clinic, environmental factors also seem to play a role. In fact, many psoriasis sufferers find that certain factors will trigger an outbreak or worsen one that is already underway.
The physical component of dealing with psoriasis ranges from mild disruption to severe disruption of daily life. Psychological complications are not unusual, especially when the condition is readily visible to others, as can happen with scalp psoriasis. Some people suffer from depression, stress and anxiety as a result. They may withdraw to escape the social stigma that outsiders at times attach to the condition.
Normally, skin cells go through a month-long life cycle. New cells are formed deep within the skin, and over a period of about 28 to 30 days they make their way to the top of the skin. By that time old skin cells die and are sloughed off by everyday routines such as showering and toweling off.
The skin of a person with psoriasis, however, goes into fast-forward. The entire skin cell process happens in three or four days, causing a buildup of dead skin cells on the surface of the skin. Thankfully, this quickening of skin cells usually happens in patches, mostly on the scalp, lower back, elbows, knees, and knuckles. The technical term for these dry, irritating, scaly patches is plaques.
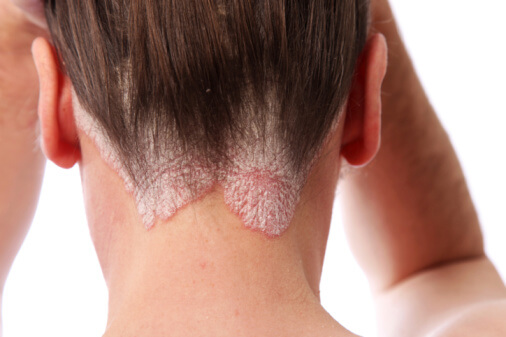
Psoriasis comes in several variations. By far, the most common type is plaque psoriasis, which is identified by its red lesions and silvery scales. Scalp psoriasis is a form of plaque psoriasis. Scalp psoriasis can consist of a single patch, multiple patches or it can cover the entire scalp. Sometimes it goes beyond the scalp to the forehead, the back of the neck or behind the ears.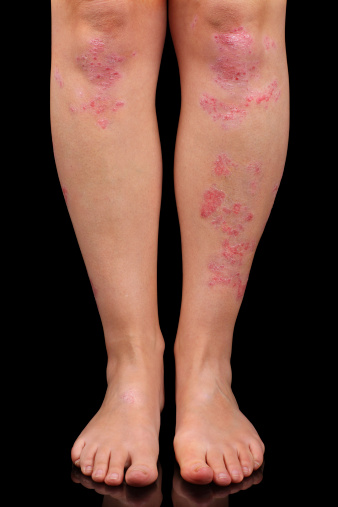
The lesions (plaque) of scalp psoriasis can be so minor that they're barely noticeable, or they can be quite inflamed and swollen. The silvery-white scales that appear look a lot like dandruff. Other symptoms are a burning sensation, temporary hair loss, dry scalp and itching. Not everyone will experience every symptom. Hair loss is usually temporary and comes from too much scratching or being too harsh in removing scales [source: American Academy of Dermatology].
Although scalp psoriasis sounds scary and can be quite unpleasant, treatments can interrupt the cycle of rapid cell growth, remove the scales and treat plaques that have formed. This article will delve into the causes of the disorder and explain medical and at-home treatments.
The following paragraphs delineate the many effective treatments devised for managing scalp psoriasis. Some people can manage with over-the-counter products. For others, prescription treatments are necessary.
It is not uncommon for scalp treatments to take eight or more weeks to get scalp psoriasis under control. According to the National Psoriasis Foundation, after it is under control, using a medicated shampoo, eating an alkaline diet and keeping stress levels at bay on a regular basis, may keep the problem from returning.
For people with mild to moderate scalp psoriasis, over-the-counter products or home remedies may work temporarily.
Found in a variety of soaps and shampoos, is frequently used to soften scales, thus making them easier to remove. Please note that long term usage may result in possible damage or hair loss; salicylic acid can weaken hair shafts, making them susceptible to breakage. However, any hair loss should be temporary.
Another great home remedy is heated olive oil or jojoba oil to soften scales. After application to the scalp, treatment consists of wrapping the head in a towel for several hours or sitting under a hair dryer, sauna or steam room. Other over-the-counter scale-softening topical medications include ingredients such as urea, lactic acid and phenol.
Both coal and, less frequently, wood— are effective scalp psoriasis treatments. Tar products come in a variety of forms, but are often seen in shampoos. The drawbacks of tar products are the strong odor and staining. Tar can stain and discolor bedding, linens, clothing and white or gray hair. The National Psoriasis Foundation suggests that tar products be massaged into the scalp and left on for a certain period of time before being rinsed off. If a tar product is used in shampoo form, try following it with a non-medicated conditioner to help eliminate the tar smell. Also, if skin is raw from itching, tar may sting quite a bit upon application, so be advised.
Either at-home or done by a medical professional (such as with an excimer laser), can also be used to effectively treat scalp psoriasis. Phototherapy can be as simple as using natural sunlight. It's also possible to use a hand-held UV comb to get light treatment to the scalp. The National Psoriasis Foundation's Web site has a database that allows visitors to search for treatments that are most effective for the scalp or other body parts. If the treatment for scalp psoriasis seems worse than the actual disease itself, please seek a dermatologist or other health care professional for changes to your treatment plan.
There are many ways people can help control and prevent flare-ups of psoriasis.
Psoriasis symptoms get worse when skin is dry, so keep it moist with creams and lotions. Thick and oily moisturizers are often the best, since they're good at trapping moisture beneath the skin. Moisturizers are also useful for removing scales, especially if you use occlusion -- applying moisturizer and then wrapping the area with tape or plastic wrap.
People with psoriasis should always be careful with their skin. Never pick at lesions or scales, since that can just make psoriasis worse. Trimming nails regularly can be a good way to prevent psoriasis from flaring up as well. If psoriasis is on the scalp, make sure that any topical treatments -- such as tar or steroid shampoos -- get on your scalp and not just your hair. Also, regular bathing with soothing products, such as tar solutions, may help.
Climate can have a big effect on psoriasis, and for a lot of people, cold and dry weather can make the symptoms of psoriasis worse. In general, hot weather is better for people with psoriasis, although some have worsening symptoms when the heat and humidity rise.
Keeping the skin moist is important. Use a humidifier during dry seasons of the year.
Tell your health care provider all the medications you take, and ask if any could affect your psoriasis.
✣ Lithium, used to treat psychiatric disorders
✣ Propranalol and possibly other beta-blockers, which are prescribed for heart conditions
✣ Cardioquin or Quinidex, medications for heart arrhythmias
If you're using any of these medications, ask your doctor about substitutes.
It is very important for people with psoriasis to avoid bumps and cuts, because trauma to the skin can cause a flare-up of psoriasis at the site of the injury, a condition called "Koebner's phenomenon." Infections can also cause psoriasis to appear. Be especially careful when shaving. Avoid insect bites, chafing, acupuncture, and tattoos.
Because ultraviolet rays in sunlight slow the growth of skin cells, getting moderate doses of sun is a good idea. However, make sure they are brief (less than 20 minutes). Use sunscreen if you are out in the sun for any longer period of time. Remember that sunburn can make your psoriasis worse, and too much sun raises your risk of skin cancer. If you're on medication that makes your skin more sensitive to ultraviolet rays as part of your phototherapy, ask your doctor about whether you should always use sunscreen when outside.
Psoriasis tends to flare up during stressful times. Try to reduce your stress levels by practicing relaxation techniques and exercising. Vedic or transcendental meditation, yoga or any other type of stress-reducing practice is great for psoriasis sufferers.
There is some research that points to alcohol as a psoriasis symptom exacerbator, at least in men. Alcohol can also be dangerous if people are using certain systemic drugs to treat psoriasis.
Many experts recommend that people with psoriasis should eat a well-balanced, alkaline, high in fruits and vegetables, avoiding refined sugars, processed foods, acidic foods and meals high in animal protein. DRINK LOTS OF WATER! Drink at least 2 liters a day. As far as foods are concerned, these are popular triggers (worsen psoriasis;) soft drinks, red wine, red meat, MSG, chili, hot spices, junk foods, oily foods, berries (such as strawberries), tomatoes, and vitamin-c. People with poor diets will likely have much worse psoriasis. Exercise may also help, and will improve your mood. In some cases, excess weight can worsen psoriasis symptoms, so maintaining a healthy weight may help prevent flare-ups.
Resources: Mayoclinic.com, WebMD.com, health.com
